What is acne?
Medically speaking, acne vulgaris is an inflammatory skin condition characterised by excess sebum (oil) production; follicular hyperkeratinisation (abnormally rapid shedding of skin cells); proliferation of the bacteria Propionibacterium acnes; and inflammation. But what does that all mean? Sebum is the oil that your body naturally produces to keep your skin lubricated; follicular hyperkeratinisation is a disorder where skin cells are shed abnormally rapidly and become sticky, which means they get stuck in the hair follicle; P. acnes is an innocuous bacterium that we all have on our skin all the time… but the problems, and the inflammation, occur when you mix those three things together. The trapped oil, skin cells and bacteria begin festering in the follicles, resulting in the skin blemishes we associate with the acne. That’s a lot of science in one sentence, but read over it until you get it, because an understanding of these elements is vital in knowing how to win the war with this condition.
When you hear talk of ‘blemishes’ and ‘spots’, those are just other words used to describe acne. If you only have a couple of spots breaking out on your face, you might think, “that’s not acne”, but to a dermatologist it’s all acne, whether you have one blemish or a hundred.
We tend to think of the acne blemishes we know all too well just as ‘spots’ or ‘zits’ but they also have quite specific definitions, depending on their characteristics:
- Comedones – these are blackheads (blocked, open pores) and whiteheads (blocked, closed pores);
- Papules – tender, little red bumps that occur when the P. acnes bacteria infection takes hold in a comedone and causes the initial inflammation;
- Pustules – papules that have become more infected and are now filled with pus;
- Nodules – large, painful and hard-to-the-touch lumps underneath the skin’s surface;
- Cysts – like nodules, but filled with pus, these are the ones that are most likely to cause scarring.
Most people will experience acne vulgaris at one point or another and, while it can be unsightly, embarrassing and annoying, it is usually something that can be effectively dealt with through good skincare and topical medications.
You may also struggle with acne mechanica, which appears at sites of increased heat and friction, for example under the band of a baseball cap. The heat and friction causes blockage of the pores, leading to comedones, papules and pustules—but not nodules or cysts.
Then there are much more severe forms of acne, such as acne conglobata and acne fulminans, which fall under the umbrella of “nodulocystic acne” and are characterised by severe outbreaks of large, thick, painful cysts, deep under the skin, some of which connect to each other in pus-filled channels. These are systemic forms of acne and require serious medical intervention, so if you think this sounds like what you’re experiencing, book a doctor’s appointment.
Acne is sometimes also confused with rosacea, but they’re different conditions (although they present with similar symptoms and have some similar causes, such as overactive oil glands). The key differences are that, with rosacea, you don’t tend to get blackheads and the skin appears to be dry and peeling, as opposed to overly oily.
What causes acne?
In the first section, ‘What is acne?’, I listed the four factors that lead to acne: excess sebum, follicular hyperkeratinisation, the P. acnes bacteria and inflammation. But what causes those factors to come about in the first place?
Hormones (specifically, androgens)
Androgens, or male hormones, cause the skin to produce more sebum (skin oil) and enlarge the sebaceous glands, where the sebum comes from. The most well-known androgen is testosterone. It is most commonly linked with male development – in fact andros is Greek for ‘man’ – so you could be forgiven for thinking that androgens, such as testosterone, wouldn’t be a factor for women, but they are. Women produce testosterone too, just less of it.
The correlation between hormone activity and the occurrence of acne is most obvious in teenagers. Hormone production ramps up during puberty and the skin often goes haywire as a result. Without androgens, the body is unable to produce significant quantities of sebum – men who have been castrated or women who have been through the menopause do not develop acne for example. In fact, during menopause, when hormone production tails off rapidly, women tend to have much drier skin.
Medication
Every prescription medication seems to come with a list of possible side effects that’s as long as your arm. Squirrelled away in the small print of certain medications, you’ll often see acne listed. The reason for this is that some medicines affect your hormone levels. But which medicines do you have to watch out for? Here are some of the more common ones that may contribute to acne:
- Contraceptives, such as the pill, injectables and intrauterine devices (IUDs), all of which work by changing hormone levels. You may be thinking, “But I’ve heard that the pill can improve your skin?” You’d be right – it can, however, side effects vary from person to person. While one brand of the pill might clear up your friend’s skin, there’s no guarantee it will do the same for you. If you’re on the pill and find that your acne has become worse, talk to your doctor about changing brands to find one you tolerate better.
- Steroids. Whether being taken as a legitimate prescription (corticosteroids) or as part of a misguided bodybuilding routine (anabolic steroids), significant steroid use makes the body think that testosterone levels are on the rise, which results in overactive sebaceous glands and more sebum production. Steroid abuse can lead to the severest forms of nodulocystic acne, like acne fulminans. If you’re considering steroid use without oversight from a doctor, please don’t do it – if you need convincing just look for images of “acne fulminans” and decide whether bigger muscles are worth the risk.
- Testosterone. This can be prescribed as a medicine to treat certain conditions and works in the same way as naturally produced testosterone, increasing sebum production and worsening acne.
Diet
There is some controversy surrounding the relationship between nutrition and acne. The traditional view is that diet can neither cause nor cure acne, and in my opinion this is accurate. However, that is not to say that diet has no effect on acne at all. There is clinical research evidencing that vitamins A and D have an important role to play in the behaviour of keratin and that fatty acids have an effect on skin conditions. Omega-3 and omega-6 imbalances are also commonly accepted to aggravate inflammation. Vitamin E is also thought to be a useful tool for inhibiting inflammation. Studies appear to suggest that people who drink a lot (ie, more than a pint, or half a litre a day) of cow’s milk, and people who eat a lot of foods with a high glycemic index, such as sugar, or white flour, have worse acne than those who don’t, but these are suggestions from a number of trials, rather than concrete facts.
Dairy, and more specifically cow’s milk, has also been linked to acne because, by its very nature, like all milk, it contains hormones. Researchers suggest that, because many cows are also now given artificial hormones too, this may affect their milk supply and in turn impact the hormonal balance of your skin when you consume it.
In fact, one study showed that women who drank two or more glasses of skimmed milk per day were 44% more likely to have acne.
However it is widely acknowledged that more research is needed into the exact reasons why cow’s milk may worsen acne. Interestingly, no studies have shown that yogurt or cheese lead to more breakouts.
Nutrition of course impacts our overall health and wellbeing, so it would be foolhardy to write off the effect of nutrition completely. Put it this way: I definitely wouldn’t indulge in unhealthy foods if I had acne. Concentrate on eating the sort of food groups that you know to be healthy – plenty of fresh vegetables, enough protein, healthy fats, wholegrains and see whether it has any effect on your skin. Look for foods that boost your levels of vitamins A, D and E and make changes to get some more omega-3 in your life, whether through supplements or diet changes. Anecdotally, people have found that cutting out foods, for example milk or sugar, has worked wonders on their acne, so why not give that a try and see whether it works for you?
Stress
This isn’t a direct cause of acne, per se, but it certainly has a role to play in making acne worse. Stress results in activity in the adrenal glands, which has the knock-on effect of increasing activity in the sebaceous glands and therefore the production of sebum. While sebum production alone doesn’t cause acne, if your skin is churning out a lot of it, it may make it more likely to kick off and break out in spots.
Heat and Friction
This is the cause of a specific type of acne called acne mechanica and occurs when something (usually clothing, or more recently face masks) is tight against the skin and rubs against it. This heat and friction leads to blockages within the pores, resulting in comedones, papules and pustules.
Is acne caused by hormones?
Yes, normal acne, or acne vulgaris, is caused by hormones, specifically androgens such as testosterone. This is why acne is so often associated with teenagers, since they are on the business end of some seismic hormonal changes, which sends the body into overdrive in many ways. Take a look at the ‘What causes acne?’ section above for more information.
Do only teenagers get acne?
If only acne was something that we could guarantee we would outgrow! Acne vulgaris is the most common form of acne and is invariably caused by hormone activity, so more often than not you see acne on teenagers going through puberty and all the hormonal changes that come with that turbulent period in our lives. However, the condition is by no means exclusively limited to teenagers. Most people who develop acne in their teens will see remnants of it in their 20s and possibly even their 30s. It is also perfectly possible for children, even babies, to suffer from acne.
Adult onset acne is also on the rise where people (mainly women) who did not necessarily suffer from acne as teens develop it in their 30s, 40s and beyond. Middle-aged women can find that the approach of the menopause and all the hormonal disruption that comes along with that, can trigger acne breakouts. When the condition is brought on by medication or you’re talking about acne mechanica, that can come at any time in your life.
Why is my skin breaking out?
If your skin is breaking out in spots then you have acne and will want to read everything on this page to understand what you can do to treat the condition over the long term. Of course there are times when acne flares up and seems much worse than usual, even if you’ve kept to your skincare routine. When you’re talking about these occasional flare-ups, there are a few reasons:
- Sudden hormonal changes. This might be due to:
- The menstrual cycle (not much you can do about this one, just wait it out and keep to your skin routine to enable it to do its thing efficiently);
- Starting a new medication (if the breakout doesn’t clear up, then the only option is to talk to your doctor to see whether this is an alternative medication you can try that you will tolerate better);
- Entering puberty (in which case, this probably isn’t properly classed as a breakout, but the start of a longer-term experience with acne);
- Drinking lots more water than you did before. I know, we’re always being told to drink more water, so why does it cause breakouts? Remember that inflammation is an essential characteristic of acne. The inflammation is actually the body’s T-cells (immune system) fighting the bacterial infection caused by P. acnes, which results in redness, swelling and tenderness. Water helps the body to work more efficiently, so when you increase your intake, your body is able to produce and send more T-cells out to tackle the acne, resulting in a flare-up as the battle intensity rages. If you’ve ever tried the sort of detox regime that involves drinking loads more water, breakouts often follow, which seems very unfair. Some people see this as the body ‘purging’ itself. Don’t worry, it’ll be over in a few days and your skin will thank you for continued hydration— so keep drinking that water.
- New environmental factors. A new perfume, shampoo or laundry detergent can sometimes be the culprit. If it is, you’ll want to eliminate the new product from your life as it will keep on irritating the skin and causing breakouts.
- Using the wrong skincare products. Think about anything you have introduced to your routine in the last few weeks, particularly anything that’s either very drying, or too heavy and oily. Products that dry out the skin give great results initially, but can cause the body to kick up the sebum production to a whole new level, resulting in oilier skin and worse acne than ever. Heavier, oilier products can simply make the pores clog further.
- UV exposure. Many people believe that the sun is a cure for acne but, while a little bit of sun can be good for us, and may have a temporary effect on the appearance of acne, it is certainly not a viable cure. One of the reasons people think the sun cures acne is that in the short term it can mask the redness associated with acne as your skin colour changes and tans. The sun also dries out your skin but this is only going to cause more sebum production further down the line. Sunshine also suppresses the immune response – in this case, the inflammation in your skin – so acne looks better in the short term, but that immune suppression is also laying your skin more open to UV damage and the problems it can bring, such as accelerated skin ageing and skin cancer, in future. So make sure you always wear protection and if you have acne-prone skin, stick with a lightweight, oil-free sunscreen.
- Stress. Something like starting a new job, going on a date (we’ve all had that unwelcome whopper of a blemish appear in the middle of our faces prior to a first date), or anything that has the capacity to preoccupy your mind is going to ramp up your stress levels and potentially lead to a breakout.
- Dietary changes. Have you recently cut something out or started having more of something in your diet? While nutrition doesn’t cause acne, it is thought to have an effect on it, so think about what you’ve been eating and you might find the cause of your breakout.
These are the most common factors, but any change can affect your skin health, so the best advice is to give careful thought to what has changed in the last few weeks. If you can narrow it down to one thing, that’s probably what led to the breakout.
Why do I have acne on my chin?
You have more sebaceous glands on your chin than on other parts of your body, and they’re larger, too, which is why your chin can be a hotbed for acne. If this happens, you’re most likely suffering due to hormonal changes. These might be age-related hormonal fluctuations during puberty, side effects from medicine, the consequences of being on your period or the onset of the menopause.
How do I prevent acne?
Cleanse your face regularly; don’t over-exfoliate; keep your hair clean; try not to touch your face/skin too much (fingers are always laden with bacteria, and touching your face just spreads these about); wash your pillowcase regularly; do not hold your phone against your face the whole time; try to avoid makeup during breakouts and when you do wear makeup make sure you clean your brushes regularly. Bear in mind that acne is hormonally-driven and you can’t prevent your hormones from doing what they do, so if you are suffering with it, get professional help, preferably from a qualified dermatologist
How can I treat acne?
You can treat acne vulgaris using a skincare regime, which I’ll talk about a little later. This should clear up milder cases of acne to the point where you only have to worry about keeping up the routine and dealing with the occasional blemish that defies the odds to make it to the surface.
If skincare isn’t working, or isn’t completely clearing up your skin, it’s likely you’ll need to supplement your regimen with some professional intervention. You can go down the route of antibiotics, although they can carry unwanted side effects, such as increased resistance to antibiotics further down the road and heightened sensitivity to UV rays – someone I talked to came out of the sun red-raw after 10 minutes when on antibiotics for acne, even though he’s Greek and had never burned in 22 years before that. Instead, you can opt for tweakments which target the elements that characterise acne. Here are a few suggestions:
Skin peels — If anything is going to clear your pores of all the dead skin cells and what have you that lead to comedones and spots, it’s a good skin peel. By using acids to exfoliate the skin, soften the heads of comedones, and (if they use salicylic acid, which they should) get into the pores to clear them out, you can leave your skin clean and clear. Be careful, though, if you’re in the middle of a breakout. If your skin is especially sensitive, skin peels can have an adverse effect. Wait until your skin has settled down a bit before going down this road.
LED Blue Light Therapy — this tackles the P. acnes bacteria, minimising the chances it can cause the inflammatory reaction that results in pustules and cysts. There’s also evidence to suggest that LED Red Light therapy can help with hyperkeratinisation, so try both and see what works best for you.
INTRAcel — a combination of microneedling and radiofrequency that not only tightens the skin, but reduces sebum production, too. If you’re suffering with acne in later years, this is a great combination treatment that helps you mitigate the signs of ageing whilst tackling blemishes and redness.
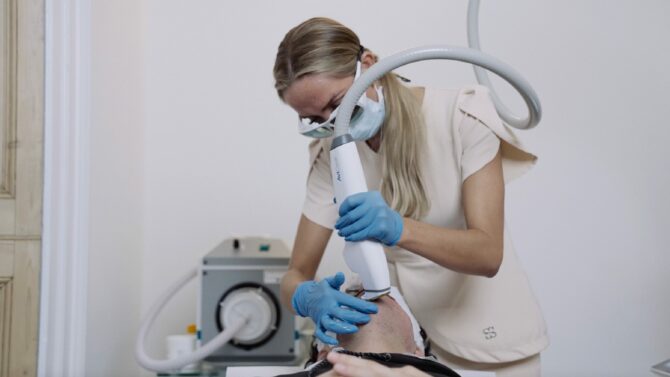
Laser Facial – The power of laser knows no limits when it comes to skin concerns. One of its lesser-known superpowers is its ability to clear up acneic skin and deal with the aftermath, too. The body stimulates a healing process inclusive of the production of new collagen, elastin, and healthy skin with often little downtime. This style of laser is also fantastic to combine with peels for optimal results.
Can I use skincare to treat acne?
Yes you absolutely can, but it is really important to understand the science behind acne, so you know how to treat it effectively. First off, skincare is often effective for acne vulgaris and acne mechanica, which is what affects most people. However, if you’re at the severe end of the scale and experiencing nodulocystic acne, then skincare will likely be pretty ineffective, although it will still be good practice as it should help the condition from worsening. Also, if your acne has come about due to medication or is getting worse due to diet and/or stress, then that’s where you need to make the change—skincare can only do so much.
If you’re suffering from acne then you need to ensure that the term ‘non-comedogenic’ is prominently displayed on all skincare and make-up that you use. Non-comedogenic just means that it won’t block your pores. Surprisingly, a lot of high-street skincare and make-up isn’t non-comedogenic, so make sure to do your research.
With acne, your skin is inflamed, so you want to be delicate with it. And patient. Some skincare is effective because it is very drying, however, those good results tend to wear off once the body starts to readjust, either landing you back at square one or, sometimes, with even worse skin that when you started. Instead, you want to adopt a gentle approach to slowly encourage your skin back into line. This will provide long-term equilibrium and it’s good practice for good skin health.
The four essential steps are:
- Cleanse – everyone needs to cleanse their face. Think about it, if your skin is clean, there’s less to block the pores, so this is always going to be a good place to start. During the day, a certain amount of grime, bacteria, sweat and oil accumulates on your skin, so you need to clean that away in the evening. In the morning, it’s good to clean the skin of the sebum and sweat that has been produced overnight. Cleansing will also make sure that any treatment products you use are going to sink in and take hold.
- Treat — as in, use a treatment product that will tackle acne. In the morning:
- The first thing I’d suggest would be to use salicylic acid, which usually comes as a runny lotion, which you can put onto cotton wool and wipe over your face. Salicylic is a beta-hydroxy acid (BHA) – the only beta-hydroxy acid – and it is ‘lipophilic’ which means that it can dissolve its way through oil. It also has a mild exfoliating action. This means that it can sink into your blocked pores and clears them out from the inside. It is anti-inflammatory, too, which helps to calm spotty skin.
- Or, you could use an alpha-hydroxy acid (AHA) product, such as an ‘acid toner’ containing either glycolic acid or lactic acid. These are both AHAs, and exfoliate the surface of the skin by dissolving the bonds that are keeping old dead skin cells glued to the surface. That means that AHAs are good at softening the top of comedones and other spots. Which to choose? Start with lactic acid, as it is gentler than glycolic acid.
- Another acid that may be worth trying is azelaic acid (a dicarboxylic acid), which helps to reduce redness and inflammation in the skin, and reduces the overproduction of keratin (which is what is contributing to blocking pores and creating acne).
- You could try products containing benzoyl peroxide, an ingredient which goes after the P. acnes bacteria, like azelaic acid does, but is more aggressive and has the added drawback of bleaching your pillows at night if you’re not careful. However, it’s cheaper and effective if your skin tolerates it well.
NB. Use one or the other of these – don’t use all of them at once, unless you’ve chosen a combined ‘alpha-beta’ solution which puts options (a) and (b) together in a tolerable way. At night:
- Use a treatment product containing retinol. Retinol is derived from vitamin A and is the closest skincare has to a miracle ingredient. It helps to normalise the skin. If you’re prone to breakouts, it can help by reducing skin oiliness, encouraging the turnover of skin cells so as to keep the surface exfoliated and stimulating the formation of collagen and elastin in the deeper layers of the skin, and reducing the hyperkeratinisation which makes the follicles block up. Is there a catch? Only in that you need to use products containing retinol, or other ingredients derived from vitamin A, with caution, and allow your skin to adapt to it. That means once or twice a week at first, then every other day. Go too fast with it, and your skin may become dry, red and flaky, so take your time.
- Hydrate – ie, moisturise! When your skin is oily, you might think that drying it out will help reduce spots. But even if it is oily, your skin still needs moisture, in the form of water, to function properly. So, while reducing oil production (with retinol, for example) is helpful, you don’t want skin to be dehydrated and short on moisture. Pick a hydrating serum or moisturising gel with ingredients like hyaluronic acid and glycerin, which will draw water into the skin and help keep it more comfortable. Choose one that is oil-free.
- Protect – ultraviolet light, i.e. normal daylight as well as bright sunlight, does your skin no favours, so in my opinion, you should be wearing a sunscreen product every day of the year. If you are using retinol or a prescription vitamin A product, sunscreen is even more vital as it makes the skin more sensitive to light. If you have acne, you may well have a horror of thick, gloopy sunscreens that feel like they’re clogging the skin and making everything worse, but there are many products that are lightweight, oil-free, and which will give the skin good protection without aggravating acne.
There are some other products you’ll often see in acne-specific skin regimens, which I’ll address here as well:
-
-
- Scrubs – with acne, you really don’t want to irritate the skin with anything overly aggressive. Scrubs sound like a good idea in as much as they can help to slough off the dead skin cells and keep the skin’s surface clear, but I prefer chemical exfoliants, i.e. salicylic acid and alpha-hydroxy acids, as mentioned above. These will provide plenty of exfoliation without scratching away the surface of the skin or irritating blemishes further.
- Skin peels – we’re talking about at-home peels here, not ones performed by a practitioner. AHAs and BHAs are often present in skin peels: the former will exfoliate the outer layer of the skin and soften the tops of comedones, the latter gets into the pores and cleans them out from inside. They’re great ideas in principle, but remember you want to be gentle to skin that’s suffering with acne. Too harsh a peel done too often will not help, so tread very carefully.
I mentioned above that it can take eight weeks from the formation of a comedone to the appearance of a papule or pustule, so there’s no quick fix for this. Working out a skincare regime that works for you involves a bit of trial and error, and it will take a while to judge whether something you’re doing actually is an error. Stick at it, be consistent, don’t change products for the sake of it, and chart your progress. Be intelligent in your approach and use all the information on this page to work out which products are likely to work for you.
Does the pill help with acne?
Yes, some types of contraceptive pill can improve acne. Some brands of the pill contain a chemical called ethynyloestradiol (EO) which raises the levels of a substance called sex hormone binding globulin (SHBG) in the body. That’s useful because SHBG is the ‘binding protein’ for free testosterone – the type of testosterone that provokes your oil-producing glands into overreacting, so it fastens on to the free testosterone and makes it harmless.
Other ingredients which are combined with EO in birth control pills which can be helpful for acne sufferers include levonorgestrel, norethindrone, norgestimate, drospirenone, cyproterone acetate, chlormadinone acetate, dienogest or desogestrel.
Which pills? Yasmin and Dianette are two of the best-known.
Is there a natural treatment for acne?
We all love a natural skin hack, but when it comes to acne you have to be so careful not to do anything too aggressive. That’s why things like tea tree oil and lemon juice are such a bad idea. They’re highly astringent and will therefore dry out your spots, but they go way too far in the other direction, leaving your body concerned that the skin is dehydrated. What does the body produce to hydrate the skin? You guessed it: sebum! The one thing you really don’t want more of when you’re treating acne. The same applies to witch hazel and rosewater toner, they just dry out the skin. It leads to short-term positive results, but soon your skin catches up and you’re back to where you started, just with more sebum to contend with.
While I wouldn’t recommend any natural products, there are certain lifestyle changes which will help:
-
-
- Drink lots of water – you might find this spurs a breakout to start with, but after 10 days or so your skin will be so much more hydrated, so the body will produce less sebum;
- Sleep well – sleep is vital for regulating our body’s processes, including moisture dispersal and skin cell regeneration and turnover;
- Bring your stress levels down – stress aggravates acne, so take time to achieve balance, meditate twice a day and centre yourself to bring that adrenaline down;
- Eat healthily – focus on vitamins A, D and E (more on this above). Vitamin A can be found in dark green leafy vegetables, orange and yellow fruits and vegetable; vitamin D in oily fish, cheese and egg yolks; vitamin E is found in nuts like almonds, hazelnuts and peanuts. (You can get vitamin E from vegetable oils, but they’re also high in omega-6, something you want to consume less of, not more.) Omega-3-rich foods include oily fish, seaweed, flaxseed and walnuts. Fruits and vegetables in general will help to hydrate your skin and boost antioxidant levels, all of which will help with acne.
Do pimple patches work?
Yes, pimple patches are a brilliant invention. These are little sticking plasters which are usually semi-transparent which can be stuck right over the top of a spot or breakout and if left on overnight can greatly reduce the inflammation in spots which are threatening to erupt, or which already have whiteheads.
They are either made with a hydrocolloid dressing on the inside, which will absorb moisture from the spot and draw out the gunk at the same time, or they have spot-busting ingredients such as salicylic acid on the inside, compressed into tiny needle-shapes that dissolve into the surface of the spot.
You need to leave these on the face for several hours, preferably overnight, in order for them to have the best effect. The other benefit of these patches is that while they are on the spot, they prevent you from scratching or picking at the spot, or even absent-mindedly touching it.
Can light treatment help acne?
Yes, certain kinds of light treatment can definitely help acne. Not the exposure-to-sunlight type of light therapy that used to be recommended by doctors in the 1950s (see above to read why that isn’t a good idea), but treatment with LED light helps acne a good deal.
-
-
- Blue LED light treatment. Lying under a canopy of blue LED lights at a clinic feels like it is doing nothing for the skin, but this light denatures the P. acnes bacteria that contribute to acne. Three sessions of treatment per week for two weeks should quieten down acne a great deal. However, because it is neither treating the hormones that drive acne, nor the overproduction of sebum, it is likely that the acne will return.
- Red LED light treatment. This is just as quiet and comfortable as blue light treatment, but works in a different way. Red light is anti-inflammatory and has a calming effect on the skin, particularly as it is often combined in treatment with near-infrared light. Both of these wavelengths help to stimulate collagen production in the skin, which will help acne scars to heal. With red light, a course of treatment usually involves two 20-minute sessions a week, for four weeks.
These treatments can be found at skin clinics and many aesthetic doctors offer them too. Or you could try a home-use LED light mask. These offer lower light intensities than the lights found in professional-quality machines, but will give results if they are used often enough – perhaps every other day, for 10 minutes – so make sure you will find the time to use it before investing in one of these.
How do I lance a spot?
So, first off, let me be clear that you really shouldn’t be disturbing your spots in the first place. They are infection sites and, by lancing (or, worse, popping) spots, you open up the infection site to the environment and the introduction for further bacteria. A spot may be unsightly, but it’s also sealed off. Poking holes in it just makes a convenient entry route for other contaminants. The squeezing action, while seeming to satisfactorily expel all the pus in your spot, actually also pushes some of the infected gunk deeper down into the pore, which can make matters much worse. Lecture over, I appreciate that most of us will sometimes find ourselves unable to resist the urge, and yes, I still pop spots when I know I shouldn’t. So, if you’re going to do it, do it properly and follow these steps:
-
-
- Check whether this is a spot that can even be lanced – basically, it has to have a white head on it that’s really close to the surface of the skin;
- If it’s just red or one of the big cystic varieties, you must promise me not to pop it as you’ll almost inevitably cause further damage, infection and even scarring;
- Steam your face or apply a warm flannel to the skin to soften the head of the spot and relax the pore;
- Thoroughly clean the spot and the surrounding area, as well as your hands and fingers, preferably with surgical spirit, aka rubbing alcohol;
- For your lance, you want the thinnest, sharpest piece of sterilised metal you can find – sterilised, prepackaged hypodermic needles are best, but they’re not too easy to come by, so you could just sterilise a needle with rubbing alcohol or boil it thoroughly;
- Wrap your fingers in tissue and slowly insert the lance across the top of the spot’s head, ideally piercing one side and coming out of the other—don’t go straight down and don’t jab, think of this as a surgical procedure;
- Remove the lance out and away from the spot and place out of reach – do not be tempted to use it again on the same or another spot;
- Place your fingers either side of the spot, press down and then gently stretch the skin apart so you’re pulling the spot taut—this can often do the job and carries a lower risk of further infection;
- If that doesn’t work, place two cotton swabs either side of the spot, press down, then gently squeeze at the root of the spot, taking a ‘little by little’ approach and working your way around the spot to encourage a little bit out at a time. Don’t pinch hard and try to get everything out in one go as you’re heading into infection territory by going that, meaning your spot could linger than much longer;
- If that hasn’t worked, then you need to leave the area alone – that pimple is not ready to pop and persevering is without a shadow of a doubt only going to make things worse;
- You should only stretch or squeeze as much as is necessary to get rid of the pus. White fluid is not infected material, so stop if you start to see that coming out, and definitely, definitely stop if you see blood coming out, as you will have already gone too far;
- Once the deed is done, you’ll want to cleanse the area again and stop further contaminants getting in, so apply a spot treatment, bacitracin, or a pimple patch.
Should I see a dermatologist for acne?
Ideally, yes you should, because as any dermatologist will tell you, acne is a common skin condition and they have many strategies for managing it, so that you don’t have to suffer with it. In the UK it is harder to find a dermatologist simply because there are not so many of them per head of the population as there are in countries like the USA. General practitioners in the UK aren’t given much training in skin conditions – which is a real shame given how many people go to their doctor with skin-related problems. But increasingly it is possible to find doctors with a special interest in dermatology and skincare, who can advise more helpfully on how to manage conditions such as acne.
How will a dermatologist treat my acne?
First, the dermatologist will examine your skin and assess the extent of your acne. They will ask you about your lifestyle and habits, and your current skincare. They will then discuss treatment options to help bring your acne under control. These might include:
-
-
- Oral antibiotics – to bring down the inflammation in the skin. These will need to be taken for a few months to take effect.
- Prescription skincare containing active ingredients such as azelaic acid, benzoyl peroxide, or retinoic acid along with specific details of how to use these.
- Oral isotretinoin, usually known as roaccutane (in the UK) or accutane (in the USA), which shrinks the oil glands in the skin and so reduces acne at the source. It is effective, but many people are reluctant to consider it, as roaccutane has a reputation for mood disturbances, particularly in people who already suffer with low mood. The latest report on this – in the JAMA Dermatology, 2019, points out that no causal link between isotretinoin and psychiatric risk has been established, and psychiatric ‘events’ reported with isotretinoin use had to be considered in the wider context of depression among patients with acne in general. People will have their own views on this, but the current trend when treating with roaccutane is for using a low dose over time, which is easier to tolerate for the skin as well as, maybe, for the mind.
Does toothpaste really help with spots?
Please don’t do this. Toothpaste is a scouring agent you scrub onto your teeth, which are protected by hardy enamel, then wash away, not a topical application to be left on your sensitive skin. This is not a clever skin hack. It feels like it’s working and will admittedly help to dry out a spot, but it will dry out your skin, too. In more serious cases, it can cause contact dermatitis and chemical burns. So, all in all, a bad idea.
Does acne go away with time?
This depends on the type of acne you have and the root cause. Acne vulgaris comes about due to hormonal changes. If those hormonal changes are due to medication, then the acne should go away within four to eight weeks after you stop the culpable medicine. If a breakout is due to your period, your skin should clear up about eight to 10 days after the first spot appears. Where it gets less certain is when you’re talking about longer-term hormonal changes, such as those that occur during puberty and which are to blame for the vast majority of acne cases. In these cases, your acne will almost certainly go away over time, but nobody can tell you the sort of timeframe you’re looking at. You could be in for anything from a year to 25 years. Accordingly, if it’s something that affects you, then don’t leave it in the hope that it will go away, because it won’t. Seek treatment and you’ll be able to keep it under control until your hormones have completely settled.
There are, of course, other types of acne, which are a little different. Acne mechanica – the one that comes from heat and friction – will definitely go away with time, provided you get rid of whatever was causing the heat and friction in the first place. Figure on about four weeks (with a good skincare routine) for your skin to balance out again. Nodulocystic acne, however, lies at the other end of the scale and requires medical intervention to bring it under control. It can become less severe with time, but it is not something you can manage without bringing out the big medical guns.









 The Tweakments Chatbot
The Tweakments Chatbot